Gut Flora and Metal
The beginning of all life on earth was the development of microorganisms. All of the processes of life which every living cell depends on to this day were originated by bacteria and other microbes. For the first two billion years of life on earth, all life was microbial. All cells began as single cells and all life forms are meticulously organized and highly sophisticated organizations of microbial life. They invented all of life's essential, miniaturized chemical systems including fermentation, photosynthesis, oxygen breathing, DNA repair systems, cellular movement and the removal of nitrogen gas from the air.
Because bacteria can routinely and rapidly transfer bits of genetic material to each other, they are capable of adapting at the genetic level very quickly. They do not need to wait for genetic mutation and reproduction in order to adapt to environmental change. Genetic recombination is a natural process of bacteria. An even faster form of change available to microbes is symbiotic alliance, the merging of organisms into new collectives.

"Why are all these conditions related? What underlying problem are we missing in our children which makes them susceptible to asthma, eczema, allergies, dyspraxia, dyslexia, behavioral problems, ADHD, and autism in different combinations? Why, when they become teenagers, do many of these children fall prey to substance abuse? Why do many of these children grow up to become diagnosed with schizophrenia, depression, bipolar disorder and other psychological and psychiatric problems?
To answer all these questions we have to look at one factor, which unites all these patients in a clinical setting. This factor is the state of their digestive system. I have yet to meet a child with autism, ADHD/ADD, asthma, eczema, allergies, dyspraxia or dyslexia, who has not got digestive abnorm-alities.... But what have digestive abnormalities got to do with autism, hyperactivity, inability to learn, mood and behavior problems? According to recent research and clinical experience -- a lot!
...Here I propose a name: Gut and Psychology Syndrome or GAP Syndrome.
...there is another group of conditions which fit in the GAP Syndrome. These conditions are schizophrenia, depression, manic depression or bipolar disorder and obsessive/compulsive disorder.
GAPS children and adults have digestive problems, sometimes quite severe. Colic, bloating, flatulence, diarrhea, constipation, feeding difficulties and malnourishment, all to various degrees, are a typical part of autism, schizophrenia and other GAPS conditions.
...Doing the endoscopies, Dr. Wakefield's team has found various stages of chronic inflammation in the gut of these children, erosions of the mucous membranes of the colon and intestines, abcesses filled with pus, ulcers and plenty of fecal compaction. In some places the gut wall was so inflamed with such enlargment of the lymph nodes, that it almost obstructed the lumen of the gut. In some ways this inflammation resembled ulcerative colitis, in some, Crohn's disease, when some features were completely unique to these autistic children. That is why this colitis was named non-specific, because it could not be assigned to any existing diagnosis. Dr. Wakefild's team called it AUTISTIC ENTEROCOLITIS.
...A well-functioning gut with healthy gut flora holds the roots of our health. And, like a tree with sick roots is not going to thrive, the rest of the body cannot thrive without a well-functioning digestive system. The bacterial population of the gut --the gut flora-- is the soil around these roots, giving them their habitat, protection, support and nourishment.
As we know, the roots of a tree, invisible, hidden, deep under the ground, play a crucial role in the well being of every branch, every twig, every little leaf of that tree, no matter how proudly high and far they may be from those roots. In the same way the diverse and multiple functions of gut flora reach in the body far beyond the gut itself."
Gut and Psychology Syndrome, by Natasha Campbell-Mc Bride, M.D.
We Still Carry Bacteria as a Part of Our Cells
We carry the descendants of the first bacteria from the oceans that learned to use oxygen in each of our cells now as our mitochondria. Long ago the mitochondria took up residence in other microorganisms providing their specialized ability to utilize oxygen for energy production in exchange for food and shelter and they are now present in nearly every living cell on earth.
But they retain their bacterial habit of multiplying by simple division, at their own times using their own DNA. This was a symbiotic alliance that became permanent. This process of symbiosis occurs throughout all life on earth. Our cells maintain an environment that is carbon and hydrogen rich, like that of the earth when life began. They live in a medium of water and salts like the composition of the early seas. We co-exist with present day microbes and harbor remnants of others in our cells.
Without nitrogen-fixing bacteria, many soils would be sterile and unable to support plant life. Neither cows or termites can digest cellulose without the microbes in their guts. Ten percent of our own dry body weight consists of bacteria, many of which we can't live without.
Photosynthesis originally began in cyanobacteria not in plants. The green plastids such as chloroplasts were most likely originally eaten but resisted digestion by some of their hosts. Their resemblance to cyanobacteria to the present is even more obvious than the bacterial nature of mitochondria. The chloroplasts have their own DNA and RNA, their ribosomes are bacterial and they have their own membrane within the cell. They divide directly in two within the cell and their DNA, RNA and protein strongly resemble those of cyanobacteria. The plastids are now dependent on their hosts but still make some of their own proteins. Plant photosynthesis is the basis of all larger forms of life on earth. Bacterial symbiosis continues within and upon us.
The Flora are as Essential as the Liver
We each have about one billion living bacteria per gram of large bowel content. This is greater than the number of people who have ever lived. This amounts to about 3 to 4.5 pounds of bacteria in the gut. Along with sheer numbers is the great variety of species present which are somewhere between 400 to 500 different types of bacteria. Nearly all of these bacteria are anaerobic which means they cannot use oxygen in their energy metabolism.
For millions of years, all life on earth consisted of anaerobic bacteria and other micro-organisms. We carry that heritage with us to this day. When considering just the known metabolic capabilities of E. coli alone, it is obvious that the metabolic functions of the gastrointestinal flora are immense and are even greater than the functions of the liver. Without the constant assistance we receive from our beneficial flora, we could not live.
In many ways, the flora can be considered as a separate metabolic organ of the body. There is much evidence that what is considered normal gut structure and function is, in fact, the combination of a complex set of interactions between the host and the microbes that colonize the gut. This includes intestinal peristalsis, absorption, as well as the composition of the intestinal cells and their growth and health. About 60% of our immune system's receptor cells are in the large intestine. 15% are in the lower part of the small intestine. This means that 75% of the body's immune system happens in the gut and is dependent on a healthy bowel flora.
Beneficial Bacteria Are Our First Defense
The entire digestive tract is coated with a bacterial layer on the surface of the intestinal walls. This provides a natural barrier to invading organisms, undigested food, toxins and parasites. The beneficial flora such as Lactobacteria, Bifidobacteria, Propionobacteria, and certain strains of E. coli, Peptostreptococci, and Enterococci, produce antibiotic, anti-fungal, and anti-viral substances that can dissolve the membranes of viruses and bacteria. E. coli is able to use oxygen and helps to clear any oxygen that may be present to create the oxygen-free environment the beneficial flora require. E. coli is only normal in the colon and lower parts of the intestine. E. coli found anywhere else in the body is a sign of gut dysbiosis.
The flora are also essential in triggering the production of a wide range of immune cells and factors in the body including neutrophils, macrophages, immuno-globulins, interferons, interleukin-1 and tumor necrosis factor. Bifobacteria are the most active in synthesizing nutrients.
About 30 different species have been identified and they are most numerous in the colon, vagina and genital areas. Protozoa, yeasts, and other fungi occur only in very low numbers in the healthy human gut. A disturbed flora both lowers immunity and weakens the barrier functions of the intestinal wall allowing a wide range of organisms and toxins to enter the blood.
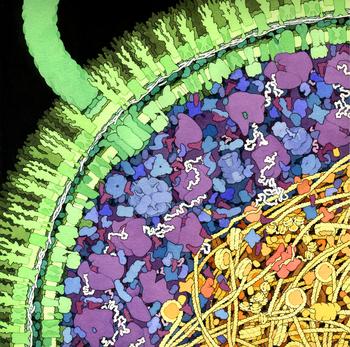
This illustration shows a cross-section of a small portion of an Escherichia coli cell. Illustration by David S. Goodsell, the Scripps Research Institute
The Specific Composition of the
Gut Flora is Mostly Unknown
There are at least 17 families of bacteria with 50 different genera. Within this are hundreds of species and subspecies. Somewhere between 400-500 is the estimated amount in a single person. The major problems with identification of the flora are the complexity of the internal ecosystem and the inaccessibility of many parts of that ecosystem in a healthy person. Getting samples from anywhere but the mouth and anus is difficult.
There are variations in the content of microbes even in different parts of the stool specimens taken. All other sampling requires invasive methods which may subject the sample to contamination. About 60% of the species are not able to be cultured in the laboratory even with excellent equipment and methods. This may be due to unknown nutritional requirements on the part of the organism, or because they must grow with other microbes that provide essential substances for them. This means they have not been studied in any detail. Methods using the identification of bacterial DNA are beginning to overcome this problem but much study remains to be done.
The beneficial flora should make up 85% of the intestinal bacteria. About 100 different kinds have been identified so far. They are primarily lactic acid producing bacteria and when they are dominant in the gut, they reduce the pH near the gut wall to 4.0-5.0. This acid environment is a strong deterrent to the growth of pathogenic bacteria and yeasts which prefer a more alkaline environment.
They are also able to neutralize a wide range of toxins both those produced by bacteria and yeasts, and those that are ingested with food and drink. They can chelate heavy metals and other poisons. A healthy gut level of the probiotics is 100 billion to 1,000 billion per milliliter of digestive tract. In many Americans today, the count is as low as 5 per milliliter. Pathogenic bacteria can include bacteroids, peptococci, staphylococci, streptococci, clostridia, yeasts, proteus, clebsielli, and many, many others.
The Flora Are Essential For Digestion
In a sterile gut such as is used in certain experiments, the intestinal walls degenerate due to the decline in cell production. The production of new cells slows down. Less cells are produced and their development is disturbed which can lead to cancer. The intestinal villi degenerate and can no longer break down and absorb food properly resulting in malabsorption, nutritional deficiencies and food intolerance.
In addition to protecting and nourishing the intestinal wall itself, the beneficial flora take an active part in digestion and absorption. The flora help digest proteins, ferment carbohydrates, and break down fats and fiber. Bacterial by-products are important in absorbing minerals, vitamins and many other nutrients through the gut wall. In addition, the flora produces many vitamins including vitamin K, pantothenic acid, B1, B2, niacin, B6, and B12. This keeps the body's supply of these nutrients steady. Normal digestion and absorption of food is probably impossible without normal flora. Certain foods cannot be digested at all without it such as fiber and lactose.
Fiber is an important food for the beneficial flora. They feed on it providing nutrition for the gut wall, and the body. The fiber is primarily broken down into short-chain fatty acids (acetic, propionic and butyric acid) and carbon dioxide. In omnivores such as humans these acids are produced throughout the large intestine. These fatty acids supply 50-75% of the energy requirements of the cells of the large intestine, but only about 5% of the overall energy required by the body. In ruminant animals such as cows and horses it may supply 35 – 75% of the energy for the animal.
The short chain fatty acids are converted to acetyl coenzyme A and other forms of coenzyme A either in the gut lining or the liver. Coenzyme A is then converted to energy in the mitochondria or used to make fatty acids in the cells. The bacterial action on dietary fiber allows the fiber to absorb toxins, recycle bile acids and cholesterol, and take part in electrolyte and water metabolism. The beneficial flora work on the fiber and if they are not present, it will be taken over by the pathogenic bacteria which produce toxins that cause illness and inflammation. This is what is happening when a low fiber diet is recommended for intestinal problems. Without the beneficial flora, fiber can become a source of disease.

Pathogenic Flora Compete For
Nutrients and Promote Toxicity
Anemia can be worsened by gut dysbiosis (imbalanced gut flora). When the beneficial flora are weak or absent and the pathogenic bacteria (such as actinomyces, mycobacterium, E. coli, corynebacterium and many others) are dominant, they consume any free iron available from the food being eaten. Supplementing iron in the absence of beneficial flora actually makes these pathogenic bacteria stronger and can result in many gastrointestinal side effects from the iron supplementation. An abnormal flora results in many nutritional deficiencies and promotes widespread degeneration.
The iron-binding protein transferrin is also the major aluminum-binding protein in the blood plasma, and through its binding to transferrin, aluminum can enter the brain. Iron absorption is controlled by the status of the body iron stores. The lower the body iron stores, the larger the percentage of ingested iron that will be retained in the body. The same absorptive mechanisms that increase iron uptake are involved in the uptake of lead, aluminum and cadmium. This is why an iron deficiency will worsen lead poisoning.
Pathogenic flora strongly promotes iron deficiency and an
iron deficiency increases the absorption of toxic metals into the body where
they will cause a wide range of toxic effects. When the available iron is
low, transferrin easily carries molecules of aluminum into the cells
along with whatever iron there is. Aluminum is closest in size to iron
and magnesium and will compete with them in the body.
Iron Is Essential For Proper Detoxification
Iron is required for the production of the heme proteins including hemoglobin – the red blood cells, and myoglobin. Iron is also essential for the production of another type of heme protein, the cytochrome proteins. The cytochromes of the mitochondria are used in the respiratory chain for energy production. The cytochromes of the endoplasmic reticulum include the Cytochrome P450 enzymes.
Cytochrome P450 is a group of Phase I detoxification enzymes which are essential to the first step in the detoxification process which converts toxins to a water soluble form that can be excreted. This includes drugs, pesticides, carcinogens, alcohol, and non-nutritive compounds found in plants.
A reduction in the Cytochrome P450 enzymes can cause multiple chemical sensitivities because even small amounts of toxins can result in damage throughout the body. Iron deficiency will reduce energy production, and oxygen uptake, impair detoxification and increase the absorption and retention of aluminum, lead and cadmium. This can all be caused or worsened by a pathogenic flora which consumes the iron available from food.

Aluminum Strongly Competes with Magnesium
The toxicity of aluminum usually results from inhibition of magnesium dependent enzymes as it can readily replace magnesium in biological systems because of its much higher affinity for the substrates involved. Even tiny amounts of aluminum can compete with much larger quantities of magnesium. But the enzyme action of aluminum is much slower than magnesium thereby reducing enzyme functions. Nearly all enzymes that require ATP use it in the form of Mg-ATP complex.
Interference with these enzyme pathways affects the neuromuscular functions, and the glycolytic pathway which produces energy from sugar. Magnesium is also required for the synthesis of DNA, RNA, protein, fats and carbohydrates and it plays a structural role in cell membranes, ribosomes and chromatin. It is essential for energy production in the mitochondria.
Aluminum is a very common metal in the environment and is widely used as a food additive, antacid, in deodorants, and in packaging and cookware. Disturbed bowel flora can greatly increase the absorption and toxicity of aluminum.
Low Hydrochloric Acid
Production Weakens the Flora
Low hydrochloric acid production has many negative effects on the body including an increased risk of pneumonia and other infections such as salmonella and osteoporosis. Hydrochloric acid kills most of the pathogens present in the food being eaten including parasites. Low hydrochloric acid leads to poor absorption of many nutrients. Many nutrients such as calcium and iron, amino acids and numerous vitamins depend on HCl for absorption. Low levels can also reduce liver and pancreas enzyme production and function.
Stress, over eating, drinking cold drinks with meals, eating too much protein at once, poor chewing, low zinc and iodine, chlorinated water and other factors will lead to low HCl. Depleted beneficial flora, and low hydrochloric acid will usually result in reduced digestive enzyme production and will result in creating an overly alkaline intestine which favors pathogenic bacteria and yeast.
Various forms of metal
toxicity can also interfere with the production of hydrochloric acid as it is a zinc dependent function of the body. Many toxic metals block or disturb zinc availability including mercury and cadmium.

Copper Toxicity Reduces Hydrochloric Acid Production
Hydrochloric acid production requires the presence of sodium and potassium chloride which are converted in the stomach to hydrochloric acid. Copper toxicity is an important cause of reduced HCl. This is because copper imbalance causes slow oxidation due to copper's ability to raise calcium levels in the tissues. As the metabolism slows down, the sodium and potassium levels in the tissues decline and hypo-acidity occurs.
Slow oxidizers usually have an overly alkaline intestinal tract and are very prone to yeast infections. Copper toxicity is often due to zinc deficiencies and the accumulation of toxic metals that will replace zinc such as mercury and cadmium. Slow oxidizers retain metals very easily due to the sluggish metabolism that makes it harder to excrete them. Prolonged adrenal stress is a cause of zinc loss as is over-eating sugar and using stimulants. As zinc declines, copper rises. Metal toxicity can be both a cause and an effect of adrenal stress.
Copper toxicity is a condition where there are high levels of copper building up in the body tissues, but the copper is in an unbound state and is bio-unavailable to the body. This causes simultaneous toxicity and deficiency. Copper is essential for the control of all types of fungi and yeasts throughout the body. Copper toxicity also impairs thyroid function which makes the body more vulnerable to yeast.
When a high intake of sugar or alcohol is present, zinc is rapidly lost, promoting a copper rise. In addition, yeasts and pathogenic bacteria thrive on sugars of all kinds. If the gut flora is very disturbed, any type of carbohydrate foods could promote the growth of yeast and pathogenic bacteria. When dysbiosis is present, sugar and alcohol must be completely eliminated from the diet, at least for a while.

Heavy Metals and the Flora
The effect of heavy metals on bacteria is quite variable. For many the effects are the same as they are for cells in the body such as blocking uptake of needed nutrients, substituting for them in the cell metabolism, creating more free radicals, inactivating enzyme functions and so forth. Some bacteria have developed the ability to block heavy metal absorption, rapidly excrete heavy metal or bind the metals in the cell in ways that deactivate their toxic effects. Due to the lack of full knowledge of the bowel contents and of the exact effects of metal on the millions of bacteria, it is hard to say what effect ingestion of heavy metal has on the flora in any specific way.
The toxicity of metals in the gut are strongly moderated by the presence of metallothionein. Metallothionein is involved in many functions of the body, including immunity, brain and gastrointestinal tract maturation, and the regulation of metals. Metallothionein is essential for maintenance of the proper ratio of copper to zinc. So much so, that a zinc/copper imbalance is the main indicator for a metallothionein malfunction. The malfunction could be due to a genetic weakness but may also be primarily induced by nutritional deficiencies and imbalances. The primary nutrient needed in the formation of metallothionein is zinc.
Therefore, metals that compete with zinc such as mercury and cadmium will eventually disturb metallothionein function. Metallothionein is crucial to the body in regulating and coping with toxic metals. It envelopes metals such as mercury, lead and cadmium, binding with them and carrying them out of the body. Mercury or lead in the gut require metallothionein in order to disable the toxic substance.
When mercury is ingested in any form, it produces destructive changes in the mucous membrane linings of the gastro-intestinal tract. It enters the blood circulation, travels to the tissues, and then damages literally every cell with which it comes into contact. Mercury has a long history of use as a disinfectant, and antibiotic. It is still used as an antibacterial preservative so it is certain that it would kill at least some of the flora. Ideally, ingested mercury is bound to metallothionein and transported out of the body through the bile and through the kidneys.
Without the effect of metallothionein, the toxic metals will interact with chemicals called sulfhydral groups. A combination of sulphur and hydrogen, these groups have tremendous power to bind to mercury, lead, and cadmium but especially mercury. Among the sulfhydral groups in the intestines are the enzymes that break down casein and gluten. Toxic metals and low zinc interfere with the enzyme functions giving rise to gluten intolerance to grains such as wheat, rye, barley and oats, and to dairy intolerance.

Daily Consumption of Probiotics Is
An Ancient Practice for Health
The use of probiotics is an ancient practice thousands of years old. All over the world people have used lactic acid producing bacteria to ferment milk, fruit and vegetables, beans, fish meat and cereal. Fermented foods taste better, are easier to digest and keep longer.
Sauerkraut, sourdough breads, salami, olives, yogurt, kefir, cheeses, soy sauce, miso and fermented grains are still eaten all over the world. Lactobacilli are a large family of bacteria that are essential inhabitants of the gut, mucous membranes throughout the body, and are present in large numbers in human breast milk.
Probiotic spores have been shown to be a crucial part of the gut flora. These bacterial strains are very common in people who live
close to nature such as hunter/gatherers, yet they are nearly absent
from city dwellers. They nourish your own good flora.
Drugs of all kinds, chlorine, sugar, alcohol, heavy metals, toxic chemicals, nutritional deficiencies and immune deficiencies all deplete the beneficial flora and favor pathogenic organisms. Because of this constant toxic exposure, everyone needs to constantly promote the health of the flora.
To restore and keep the tremendous health benefits of a healthy flora, the use of probiotic supplements,
probiotic foods, and pre-biotics which feed the flora such as fiber and
inulin along with the avoidance of toxins of all kinds must be a lifetime process.
Re-establishing a Healthy Flora
Correcting gut dysbiosis requires an aggressive program of no sugar from any source including fruit, and a low carbohydrate intake combined with increasing the levels of beneficial flora with probiotic supplements as tolerated. Various herbs and other substances kill yeasts and pathogenic bacteria such as garlic supplements of all kinds. Although eating garlic is always a good idea, supplements are required for an effective result when fighting infections and over-growths of pathogens such as candida.
The most effective herbal treatment I have ever found for the control of candida and the restoration of good health after years of dysbiosis is a Chinese herbal formula called Health Concerns Phellostatin. This product must be used very cautiously at first as it is very effective and can cause significant discomfort due to the toxic effects of die-off of the pathogens in the gut if the dose is too high.
It is best to work up to a high dose of probiotics and garlic supplements, and make sure sugar is completely out of the diet before attempting to use Phellostatin. It will not only kill pathogens, it will help the body heal from the damage caused by candida overgrowth.
Just Thrive or Mega Sporebiotic are the best probiotic
formulas to rebuild the beneficial intestinal flora. The probiotic
spores survive the digestive tract 100%, unlike other probiotic
formulas.
They garden the gut, killing off the bad bugs
and feeding the good ones. They nourish the gut lining, help digest
food, make antibiotics that kill candida and pathogenic bacteria
strains, feed your own good flora, and produce vitamins -- including
beta-carotene and Co-Q10. They can improve mood issues and train the
immune system of the gut improving auto-immune and immune deficiency
issues. Excellent for irritable bowel conditions.
They are particularly helpful for SIBO and candida. Start at a low dose, 1/4 to 1/2 capsule every other day, as die off will happen fairly strongly at first for most people. Work up to the full dose of one capsule per day. A sugar-free diet is essential when clearing candida and gut infections.
Candida Die-Off and Detox
It is important to kill off candida slowly. Trying to eliminate it too quickly can result in severe reactions including a flare up of symptoms related to the candida infection, flu-like detox symptoms that can become debilitating, all types of digestive discomfort and even swelling of the liver as the body is overwhelmed with the release of toxins as the candida is killed. Always back off on the dose of anything designed to kill yeast whether a medication, herbal formula or other method if these symptoms occur. Mild symptoms that are tolerable and come and go are normal.
The well known and commonly available Chinese herbal formula called Yin Chao, or Yin Qiao (or Cold Snap in health food stores) is very helpful in relieving detox and die-off symptoms. It can also be used for general discomfort ranging from sore throats, insect bites, ear aches, and non-chronic headaches to poison oak and neuralgia, especially trigeminal neuralgia. It is especially helpful in candida detoxification and can be used quite freely to control the flu-like symptoms typical of candida die off.
It can be taken up to every hour at first until the symptoms begin to subside. Then just take it whenever the symptoms begin to re-occur. Taken right away and frequently during the onset of a cold, it can stop it or make it much milder. Yin Chao is very helpful for cold and flu symptoms and reduces fever. The main contraindication to high doses is loose bowels although only a few have this problem and it is usually temporary. For a few, it is just too laxative at high doses.
After a while, as the pathogens clear the system, the die-off and
detox symptoms will become mild or non-existent. The liver will be able to
handle the toxins released and no particular symptoms will occur. The reduction in toxicity over all means you will feel better and better as health is restored.